What is Bone?
Contrary to popular belief, bone is not a lifeless structure, but living growing tissue. Throughout life, a dynamic process called “remodeling” occurs in which old bone is removed (resorption) and new bone is laid down (formation). During the resorption phase, bone removing cells (osteoclasts) carve cavities into the surface of the bone, while in the formation phase, bone forming cells (osteoblasts) fill in the cavities with new bone until the bone surface is restored. Beginning in childhood and continuing throughout adulthood, bone formation normally occurs faster than bone removal, so that bones become larger, heavier, denser. In the early to mid-thirties, bone removal overtakes bone replacement leading to a net bone loss of bone tissue.
Bone Remodeling
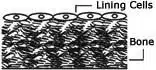 |
1. Resting Phase-A bone surface is covered by a protective layer of bone cells – called lining cells. |
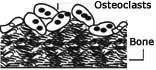 |
2. Resorption-During resorption, osteoclasts invade the bone surface and erode it, dissolving the mineral and the matrix. |
 |
3. Resorption Complete-A small cavity is created in the bone surface – resorption is complete. |
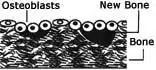 |
4. Formation Repair-Bone forming cells called osteoblasts begin to fill in the cavity with new bone. |
 |
5. Repair Complete-Finally, the bone surface is completely restored. |
How Does The Bone Function?
Bone is a specialized connective tissue that makes up, together with cartilage, the skeletal system. The human body is composed of 206 bones that perform three main functions.
1) Mechanical: Support and site of muscle attachment for locomotion
2) Protective: For vital organs and bone marrow
3) Metabolic: Reserve of ions for the entire organism, especially calcium and phosphate. Blood cell formation Storage of inorganic salts
An individual bone is composed of cartilage, fibrous connective tissue, blood and nerve tissue. Most of the bone is made of inorganic salts.
What are the parts of the bones?
On long bones, such as those in the arms and legs the large expanded portions are called epiphyses. These are the regions of the bones that articulate with other bones. The shaft of the bones between the epiphyses is called the diaphysis. Except of the articular cartilage which covers the epiphyes the entire bones is covered in a tough, vascular tissue called periosteum. Periosteum fibers interlock with fibers of tendons and muscles that are connected to the bone. The wall of the diaphysis is composed of a strong, tightly packed, bend resistant tissue called compact bone. The epiphyses, on the other hand, is formed mostly by spongy bone. Spongy bone is made of many small bone plates that have irregular interconnected spaces that help keep bones light but very strong. The compact bone in the diaphysis of long bones form a tube or channel called the medulary cavity. This cavity is continuos through the length of the diaphysis and then fades into the spongy bone. The medulary cavity is filled with a special type of soft connective tissue called marrow.
In bone, as in all connective tissues, the fundamental constituents are the cells and the extracellular matrix. The latter is particularly abundant in this tissue and is composed of collagen fibers and non-collagenous proteins. The matrix of bone, as well as the matrices of cartilage and the tissues forming the teeth, however, has a unique ability to become calcified.
Anatomically, there are two types of bones in the skeleton:
1) Flat bones include the skull, scapula, mandible, and ileum
2) Long bones include the tibia, femur, and humerus.
The osteoclast is the bone lining cell responsible for bone resorption.
What is Osteogenesis?
Bone formation (osteogenesis) begins during prenatal development and persists throughout adulthood. The bones of infants and children are softer than in adults because it has not yet been ossified (the process of synthesizing cartilage into bone).
There are two ways in which osteogenesis occurs: intramembranous ossification and endochondral ossification. Both types form by replacing existing cartilage however differ in the method they go about doing it. Two types of cells that are of great importance in the process are osteoblasts and osteoclasts. Osteoblasts, used mainly in intramembranous ossification, are the specialized cells in bone tissue that deposit calcium into the protein matrix of bone (collagen). Osteoclasts, used in endochondral ossification, dissolve calcium previously stored away in bone and carry it to tissues whenever needed.
One third of all of the bone’s components is collagen; a flexible, gelatin-like matrix. Bones formed during intramembranous formation are called membranous bones, or occasionally dermal bone, and bones formed during endochondral formation are called cartilage bone.
How does bone healing occur?
One of the most widely accepted myths about bone is that it is dead, unchanging matter. However, your bone is constantly changing every second of the day as new bone cells replace old cells, just as your dead skin cells are brushed off but are continually replaced.
The healing process of broken bones is also very similar to the healing process of skin. As soon as a bone breaks, a jacket of cells forms around the fracture (a broken bone) called a callus, in the same way skin forms a scab jacket of new cells around broken skin. Unfortunately, the callus only provides for protection from infections and such but further damage can be done if not kept in a cast. A cast is put on to keep the bone straight while healing and also it is said that by applying pressure on it the bone heals quicker. Many times the cast will be put on in such a way that you are still able to use it. This is because bone, like muscle, grows in thickness and endurance when used.
Although bone cells reproduce faster when repairing yet it still takes a long time to fully heal. In young children, while bones are still developing, repairs and healing are done fairly quickly. However as you age, healing tends to take longer. By adolescence, bones are hardened to an extent so bones are more complete. Mending in teenagers requires 6-8 weeks in a cast while after you’re 60 or over breaks occur much more easily. Sometimes just the slightest stress on a bone can break it, and then repairs are made slowly and sometimes imperfectly. However, when fractures in bone are healed with the right amount of time and nutrients to aid in it, the break or breaks in the bone cannot even be seen with an x-ray.
Tooth Extraction and Bone
Thousands of teeth are extracted annually, in the United States alone, primarily because of decay, severe periodontal disease, infection, or trauma. The jaw bone that supports the teeth, “alveolar bone”, which is generally soft and vascular, often melts away or resorbs following tooth removal. Such bone resorption can result in significant cosmetic or functional defects, including loss of surrounding gum tissue. Today, however, bioengineering has led to simple but effective surgical techniques that can either totally prevent or greatly reduce the bone and soft tissue loss that normally occurs following extraction
Tooth extraction is one of the most common dental procedures. Healing of the resulting extraction socket normally occurs uneventfully. However, even with completely normal healing, there is often some resorption or melting away of surrounding bone. Resulting in less height and width than were present prior to tooth extraction. In addition, as bone resorbs, overlying gum tissue also tends to lose both volume and its normal anatomic form. These changes can occur anywhere in the mouth but the most severe loss of bone and gum tissue tends to occur following the removal of incisor teeth located in the front of the mouth.
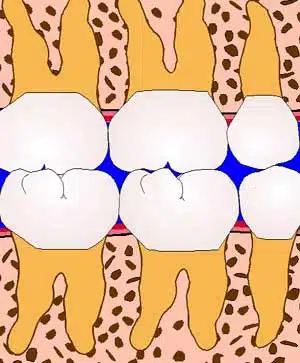
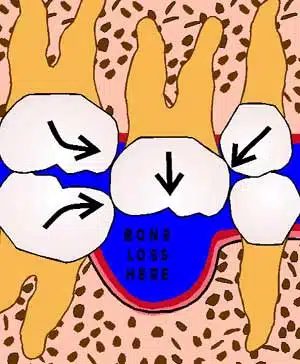
What happens to the surrounding teeth
and bone when a tooth is extracted?
Before:
After:
References:
- Medications and Bone Loss, National Osteoporosis Foundation,
- Primer of the Metabolic Bone Diseases and Disorders of Mineral Metabolism, [edited by] Favus, Murray J. Second Edition, American Society for Bone and Mineral Research. Published by Lippincott – Raven 1993.
- Bio-Oss is produced by Osteohealth Co
(A Division of Luitpold Pharmaceuticals, Inc.)
One Luitpold Drive, Shirley, NY 11967
1-800-874-2334